Blog
Cracked Heels and Keeping Feet Healthy
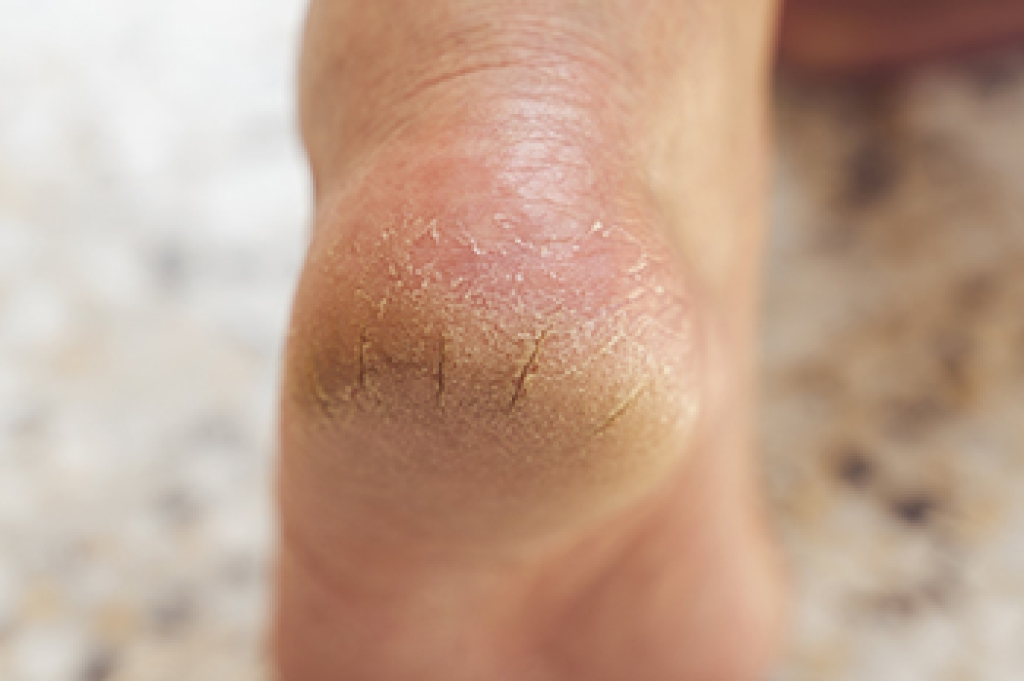
Cracked heels occur when the skin on the heels becomes dry, thick, and hardened, eventually splitting under pressure. This often develops from standing or walking on hard surfaces for long periods, which places extra stress on the heel. Being overweight can also increase pressure and contribute to skin breakdown. Symptoms include rough skin, visible cracks, and discomfort while walking. Risk factors include poor hydration, lack of foot care, and wearing open back shoes that do not provide support. A podiatrist can remove thickened skin, recommend moisturizing treatments, and provide guidance to prevent worsening of the condition. If you have developed painful cracked heels, it is suggested that you consult a podiatrist who can effectively treat this problem.
If the skin on your feet starts to crack, you may want to see a podiatrist to find treatment. If you have any concerns, contact Franklin Harry, DPM from Best Foot Forward. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
It is important to moisturize your cracked heels in order to prevent pain, bleeding, and infection. The reason cracked heels form is because the skin on the foot is too dry to support the immense pressure placed on them. When the foot expands, the dry skin on the foot begins to split.
Ways to Help Heal Them
- Invest in a good foot cream
- Try Using Petroleum Jelly
- Ease up on Soaps
- Drink Plenty of Water
Ways to Prevent Cracked Heels
- Moisturize After Showering
- Skip a Shower
- Keep Shower Water Lukewarm
- Don’t Scrub Your Feet
If you are unsure how to proceed in treating cracked heels, seek guidance from a podiatrist. Your doctor will help you with any questions or information you may need.
If you have any questions, please feel free to contact our offices located in Festus and St. Louis, MO . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ankle Sprains in Children
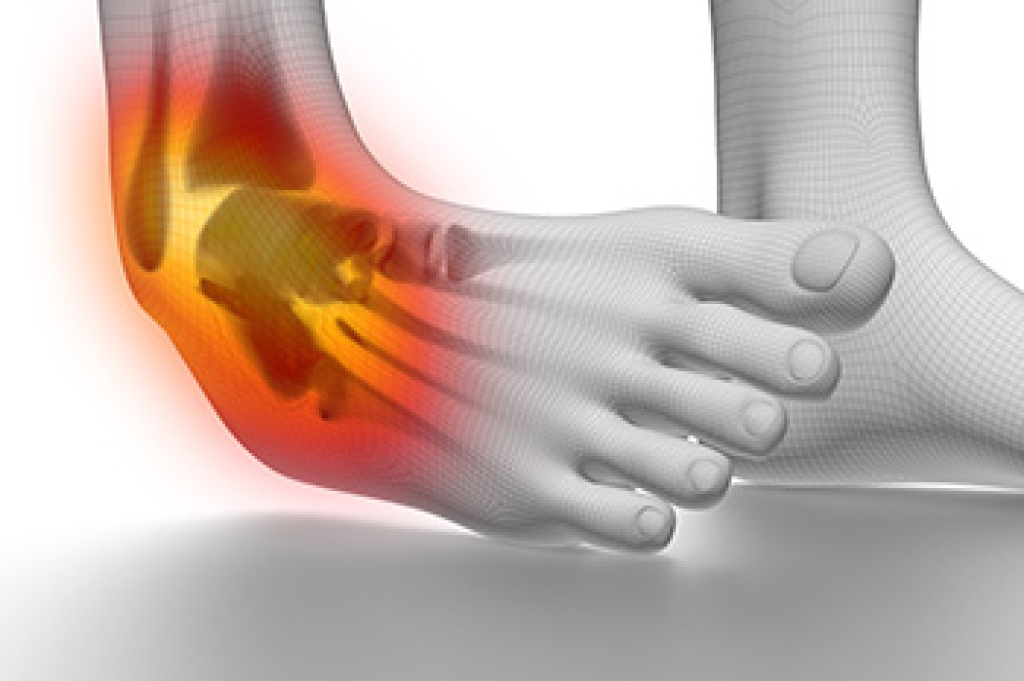
Ankle sprains are common in children, especially during sports, playground activities, or accidental falls. These injuries happen when the ligaments supporting the ankle are stretched or torn, causing pain, swelling, bruising, and trouble walking. While many ankle injuries are true sprains, some more serious conditions can appear similar at first, including growth plate injuries, fractures, or even tumors. This is why a careful evaluation is important rather than assuming the injury is minor. A podiatrist may assess the ankle through a physical examination, imaging studies, and other diagnostic tools to determine the exact cause of the pain and choose the proper treatment. Early and accurate diagnosis helps prevent delayed healing or long-term problems with stability and movement. If your child has ankle pain, swelling, or difficulty walking after an injury, it is suggested that you visit a podiatrist for effective relief and treatment solutions.
Although ankle sprains are common, they aren’t always minor injuries. If you need your ankle injury looked at, contact Franklin Harry, DPM from Best Foot Forward. Our doctor can provide the care you need to keep you pain-free and on your feet.
How Does an Ankle Sprain Occur?
Ankle sprains are the result of a tear in the ligaments within the ankle. These injuries may happen when you make a rapid shifting movement while your foot is planted. A less common way to sprain your ankle is when your ankle rolls inward while your foot turns outward.
What Are the Symptoms?
- Pain at the sight of the tear
- Bruising/Swelling
- Ankle area is tender to touch
- In severe cases, may hear/feel something tear
- Skin discoloration
Preventing a Sprain
- Wearing appropriate shoes for the occasion
- Stretching before exercises and sports
- Knowing your limits
Treatment of a Sprain
In many cases, the RICE method (Rest, Ice, Compression, and Elevate) is used to treat ankle sprains. However, you should see a podiatrist to see which treatment option would work best with your injury. In severe cases, surgery may be required.
It is important to ask your doctor about rehab options after you receive treatment for your injury. Stretching, strength training, and balance exercises may help the ankle heal while also preventing further injury.
If you have any questions, please feel free to contact our offices located in Festus and St. Louis, MO . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ankle Pain May Be Caused by Arthritis
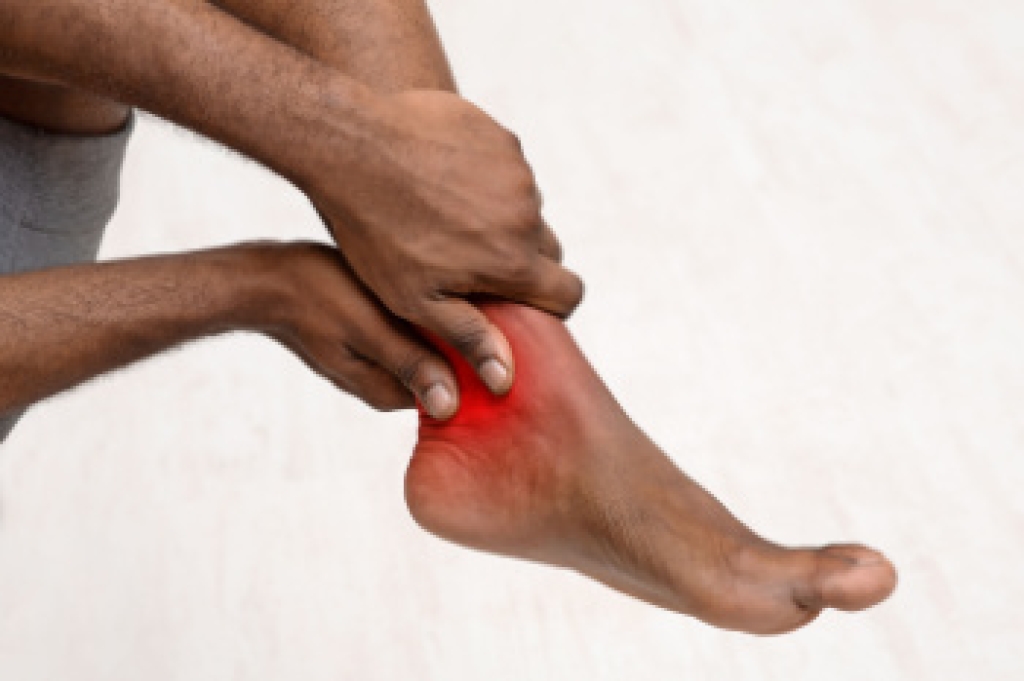
Persistent ankle pain can sometimes point to arthritis, a condition that affects the joints and limits smooth movement. Arthritis develops when the protective tissue between bones wears down or when the body’s immune system attacks joint tissue. This can lead to pain, swelling, stiffness, and reduced motion in the joint. Types of pain that affect the ankle include osteoarthritis, which is linked to joint wear over time, and rheumatoid arthritis, which causes inflammation in both ankles. Gout is another form, caused by crystal buildup in the joint that leads to sudden, intense pain. A podiatrist can examine the ankle and review imaging studies to identify the cause. Treatment plans include reducing joint stress, certain medications, and protecting the joint from further damage. If you have ankle pain, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and appropriate treatment.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Franklin Harry, DPM from Best Foot Forward. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a joint disorder that involves the inflammation of different joints in your body, such as those in your feet. Arthritis is often caused by a degenerative joint disease and causes mild to severe pain in all affected areas. In addition to this, swelling and stiffness in the affected joints can also be a common symptom of arthritis.
In many cases, wearing ill-fitting shoes can worsen the effects and pain of arthritis. Wearing shoes that have a lower heel and extra room can help your feet feel more comfortable. In cases of rheumatoid arthritis, the arch in your foot may become problematic. Buying shoes with proper arch support that contour to your feet can help immensely.
Alleviating Arthritic Pain
- Exercises that stretch the foot can prevent further pain and injury and increase mobility
- Most of the pain can be alleviated with anti-inflammatory drugs, heat, and topical medications
- Massages can help temporarily alleviate pain.
It is best to see your doctor for the treatment that is right for your needs and symptoms. Conditions vary, and a podiatrist can help you determine the right method of care for your feet.
If you have any questions please feel free to contact our offices located in Festus and St. Louis, MO . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
Plantar Fasciitis and Morning Heel Pain
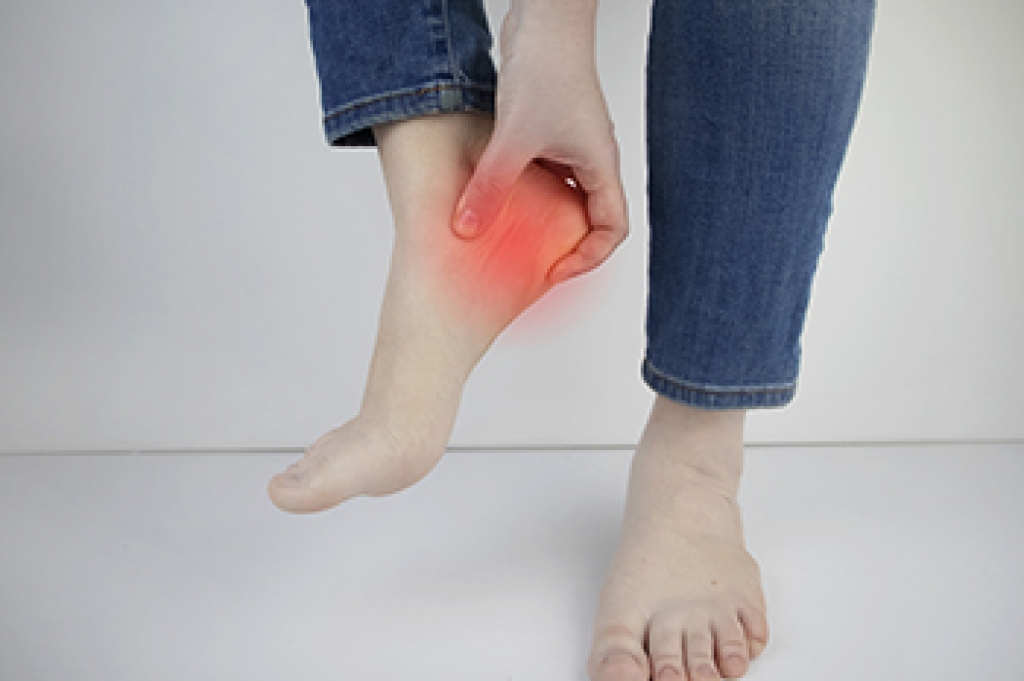
Plantar fasciitis is a common condition involving inflammation of the thick band of tissue that supports the arch of the foot. It often causes sharp pain in the heel, especially with the first steps in the morning or after periods of rest. This discomfort typically lessens as walking continues, but it may return after long periods of exertion. Pain is usually felt along the bottom of the heel and arch. Risk factors include prolonged standing, tight calf muscles, and flat feet. Having high arches and wearing shoes that lack support are other factors. Early attention can prevent worsening symptoms. A podiatrist can diagnose the condition, recommend stretching, orthotics, and other treatments to reduce strain. If you have heel pain, it is suggested that you promptly consult a podiatrist who can begin effective relief and treatment solutions.
Plantar fasciitis is a common foot condition that is often caused by a strain injury. If you are experiencing heel pain or symptoms of plantar fasciitis, contact Franklin Harry, DPM from Best Foot Forward. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is Plantar Fasciitis?
Plantar fasciitis is one of the most common causes of heel pain. The plantar fascia is a ligament that connects your heel to the front of your foot. When this ligament becomes inflamed, plantar fasciitis is the result. If you have plantar fasciitis you will have a stabbing pain that usually occurs with your first steps in the morning. As the day progresses and you walk around more, this pain will start to disappear, but it will return after long periods of standing or sitting.
What Causes Plantar Fasciitis?
- Excessive running
- Having high arches in your feet
- Other foot issues such as flat feet
- Pregnancy (due to the sudden weight gain)
- Being on your feet very often
There are some risk factors that may make you more likely to develop plantar fasciitis compared to others. The condition most commonly affects adults between the ages of 40 and 60. It also tends to affect people who are obese because the extra pounds result in extra stress being placed on the plantar fascia.
Prevention
- Take good care of your feet – Wear shoes that have good arch support and heel cushioning.
- Maintain a healthy weight
- If you are a runner, alternate running with other sports that won’t cause heel pain
There are a variety of treatment options available for plantar fasciitis along with the pain that accompanies it. Additionally, physical therapy is a very important component in the treatment process. It is important that you meet with your podiatrist to determine which treatment option is best for you.
If you have any questions, please feel free to contact our offices located in Festus and St. Louis, MO . We offer the newest diagnostic and treatment technologies for all your foot care needs.